Moore’s Law and The FUTURE of Healthcare
By Wayne Caswell, Founder of Modern Health Talk

This article examines a future driven by Moore’s Law and the trend of circuits and components getting smaller, faster and cheaper exponentially over time and the eventual blending of science and technology (INFO + BIO + NANO + NEURO). I approach this topic from the unique perspective of an IBM technologist, market strategist, futurist, and consumer advocate. See About the Author and About Modern Health, below, to better understand what shaped this view of the future. You can also see my slide presentation and related articles & infographics at the bottom.
Which Future?
Having a Futurist Mindset is not just about believing our best days are ahead, but having the courage to signal alarms when the path we’re headed in is dangerous or counter productive. The value of a futurist is not just in extrapolating trends, forecasting, or predicting how long it will take for innovations to get from research to mass-market adoption. By exploring alternative scenarios, and their underlying drivers and inhibitors, a futurist can help clients develop insights to steer themselves toward a more-preferred future, deciding where to invest, who to partner with, who to hire, and more.
A futurist’s approach is often to start with a solid understanding of market NEEDS and what drives innovative solutions for them, or factors that inhibit solutions. Changes in politics and public policy, for example, can be a huge driver, with Obamacare as an example, or a huge inhibitor. That’s why I’m so interested in various healthcare reforms that accompany tech innovation.
 Demographics
Demographics
Let’s start with NEED as a driver of our healthcare future.
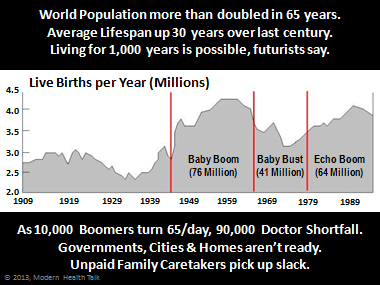
World population more than doubled in the 65 years I’ve been on the planet, from about 2.5 billion to now over 7 billion, and even though we live some 30 years longer, we’re generally less healthy. That’s largely because of technology, including electricity that allows us to work on computers in office buildings and under artificial lights. Those lights cause us to stay up later at night and interfere with our natural circadian rhythms. And the increased stress and lack of restorative sleep (1/3 get less than 6 hours/night when they should be getting 7-9) causes all sorts of health problems that seem to get worse as we age or gain weight.
Medical professionals tell us that 75% of healthcare costs go to treating chronic diseases that are largely preventable, but many of our lifestyle choices are influenced by technology. Modern architecture and transportation systems, for example, have given us easy access to food whenever we want it.
In ancient hunter-gatherer days, we might not know when we’d make another kill and eat again, so we’re genetically predisposed to eating all that’s on our plate. Our DNA has not evolved as fast as technology, so our bodies still drive us to over eat in order to store energy in case of famine. This, the lack of restorative sleep, and other factors have contributed to a population with two-thirds of adults who are overweight or obese and one third who are obese. That obesity also affects our health and contributes to rising healthcare costs.
Most other industrialized nations provide universal healthcare, but Americans rely instead on private health insurance and a for-profit system that views patients as paying customers. That system works hard to keep us coming back, treating symptoms without much regard for wellness and prevention, since that would avoid the need for medical care in the first place.
Americans spend over $3.2 trillion/year on medical care, an amount projected to reach $4.2 trillion by 2020 (or about 20% of GDP). We already spend more than twice as much as other nations in the OECD, but even with all that, we still don’t have better care. As a nation we live sicker and die younger, according to the World Health Organization.
That’s the starting point.
Next look at the 10,000 baby boomers reaching age 65 every day and the impact this aging population will have on future healthcare costs and our delivery system. We’ll soon have a major shortfall in the number of doctors and nurses to offer care, as well as a shortage of young workers to drive the economy and help pay for care.
Then there are advancements in genetic research that may soon conquer most inherited diseases, as well as therapies that repair cell damage before it accumulates. These developments will dramatically extend longevity and may one day allow people to live for a thousand years, futurists say. But at what cost?
Governments at federal, state and local levels are not ready for the coming demands on the healthcare system. Neither are the unpaid family caretakers who already spend more time caring for elderly or disable loved ones than their own children, taking time off from work, sacrificing promotions, and impacting their own health. The AARP puts the annual cost burden of these unpaid caretakers at over $480 billion per year, which is more than the $361B in Medicaid spending, and nearly as much as the $509B in Medicare spending. It will just get worse without effective tools to help.
 Technology as an Enabler
Technology as an Enabler
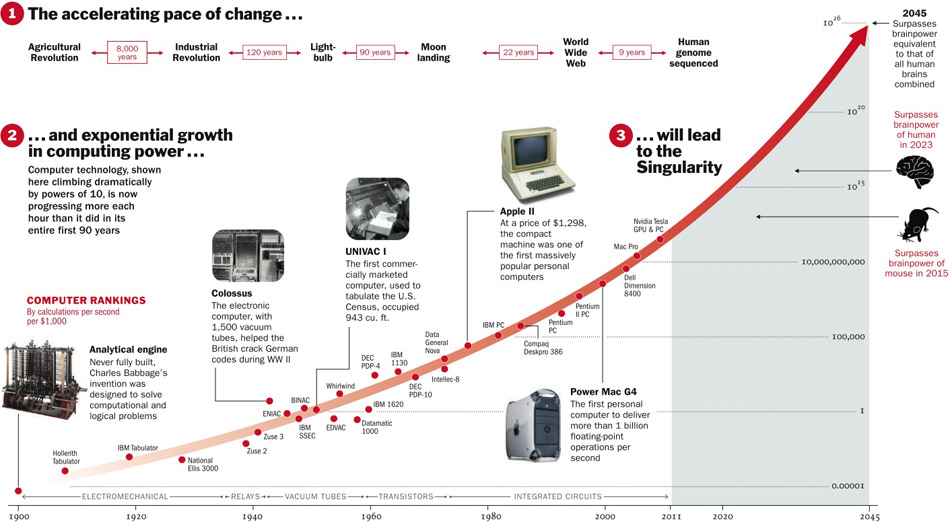
Applied appropriately, technology can provide just the right tools to help us cope with the aging population and increasing healthcare costs. It must. But public policies must change too, and embrace tech-enabled change. Fortunately, the pace of tech innovation accelerates exponentially with Moore’s Law.
I often compare today’s smartphones with one of the mainframe computers I worked on in the mid-1970s. The IBM System/370 Model 158-3 became a common performance benchmark, because it could execute 1 million instructions per second (MIPS). This $3.5 million computer was so expensive it was shared by hundreds or thousands of people. Just ten years later they all had personal computers, and each one cost 1,000 times less.
Now back to the smartphone comparison. Where that IBM mainframe was fast (1 MIPS), even the older generation Apple iPhone 4 was rated at 5,000 MIPS – i.e. 5,000 times faster than the million dollar mainframe that required a large computer room, liquid cooling, and special air conditioning. And rather than share, you carry the smartphone in your pocket everywhere you go, with the ability to sync with medical sensor devices and do Anywhere/Anytime video calls with your doctor. But with real-time monitoring of sensor data, you’ll soon have medical care Everywhere/AllTheTime.

Technology keeps getting faster, cheaper and smaller, and it’s now being embedded into everyday devices, including light bulbs, doorknobs, your clothing, and your toothbrush. For at least 5 years I’ve used a Philips Sonicare toothbrush that has an embedded microprocessor chip that’s so small and inexpensive that Philips couldn’t find a cheaper one. What I find interesting is that the processor in my toothbrush is 10 times faster than the $3.5 million IBM mainframe I worked on – my Toothbrush!
THEIR LATEST: Philips Sonicare DiamondClean 9700 Series is Everything You Could Ever Ask of a Toothbrush
 What’s next for processors and sensors?
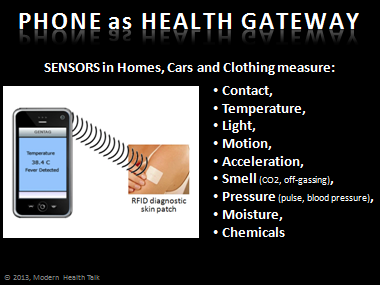
What’s next for processors and sensors?
We’ll find them in everything with a digital heartbeat, powered by electricity or not. The Philips Hue, for example, is an energy saving LED light bulb that can talk to your smartphone. Because it needs some simple electronics to convert AC current to DC, Philips added a computer chip and support for a Wi-Fi home network. As a result, you can use your smartphone to turn the light on or off, make it bright or dim, and even change its color temperature from cool blue to warm orange, which is better for nighttime and interferes less with sleep patterns.
Sensors have been used in automated homes for years, but mostly in high-end homes with professional installation, or in DIY systems cobbled together by hobbyists. With wireless networks and smarter technologies like the NEST thermostat, these sensors will gradually become mainstream – very gradually in my opinion.
As “smart” as the NEST is, it doesn’t know if I’m feeling hot because I just finished exercising or cold because I just ate ice cream. But if NEST could connect to wearable devices that sense skin temperature, it might.
I think sensors for medical applications will become mainstream faster than for smart homes, because there’s more of a need. And they’ll monitor more things. Beyond motion, light, temperature, moisture and gas; medical sensors will also monitor pressure, chemicals and biomarkers. Doctors will then be able to determine how well a drug is being metabolized and adjust the dosage and frequency accordingly.
The sensors can be in a watch you wear, on a patch on the skin, implanted under the skin, or even swallowed as part of a pill.
 Nano Scale & Macro Scale
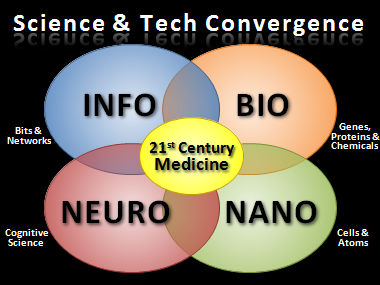
Nano Scale & Macro Scale
Consider extrapolations of Moore’s Law – where technology exponentially gets smaller, faster and cheaper – and information science (processors & networks) converges with cognitive & neuroscience (neuron signaling) and biology (chemistry, genes & proteins).
As small computer processors shrink to the size of a cell or smaller, futurists believe they’ll communicate with neurons directly. Nano-scale robots could be injected into the blood stream to seek out and destroy cancer cells. And “smart” drug delivery could deposit medications exactly where they are needed and nowhere else. But this raises new security concerns and the need for body firewalls to prevent our medical sensors from being hacked.
Moore’s Law also affects the performance of powerful supercomputers like IBM’s Watson, which is now being applied to medical diagnostics and other healthcare tasks. Watson is significant because it understands nuances of the English language and includes the artificial intelligence ability to Learn. Watson is also fast – real fast. IBM demonstrated its ability to read and analyze the equivalent of 300 million books in less than 3 seconds during a widely publicized game of Jeopardy, where Watson competed against the all time top money-winner and the guy who won the most games. Watson won.
 For perspective, if those 300 million books were stacked along a very long bookshelf, it would cover the equivalent of 7 football fields. Keep in mind that technologies that first appear in million dollar supercomputers will eventually move down-market to consumer products. The iPhone’s SIRI speech recognition software is an example since it already understands much of the English language and can carry on simple conversations. It’s not as fast as Watson yet, but watch this space.
For perspective, if those 300 million books were stacked along a very long bookshelf, it would cover the equivalent of 7 football fields. Keep in mind that technologies that first appear in million dollar supercomputers will eventually move down-market to consumer products. The iPhone’s SIRI speech recognition software is an example since it already understands much of the English language and can carry on simple conversations. It’s not as fast as Watson yet, but watch this space.
Smartphones and tablets already serve as health gateways between sensor data and powerful cloud-based services that monitor, store and analyze that data as needed. But over time more of the storage and analysis of this sensor data will occur in the mobile device itself.
Healthcare Gets Personalized & Personal
Powerful supercomputers like Watson will lead the way toward personalized medicine, doing the analytics of “big data” and helping physicians diagnose problems and personalize the medications and care plans based on a huge global knowledge base of medical information, a repository that’s doubling in size every 5 years. Such personalization will also consider the patient’s own medical record info, DNA, and monitored sensor data.
Remote access to Watson can be extended beyond doctors and will then trickle down the chain from specialists to general practitioners, physician assistants, nurse practitioners, RNs, LVNs, medical aids & techs, and eventually to consumers themselves. This will accelerate the current trend of e-patients taking more responsibility for their own health and scouring online websites (e.g. WebMD and PatientsLikeMe) for medical information about their own conditions. After all, they have more skin in the game than their physician, just not as much formal medical training.
 Telehealth & Telemedicine
Telehealth & Telemedicine
Some patients are already connecting with practitioners through high-def video calls from retail clinics or kiosks, from their home PCs (using software like Skype), or through their smartphone or tablet computer. It’s called telehealth, and new services are springing up to support it.
Your specialist and general practitioner may be miles away, but you can see and talk with them remotely; and with a few medical sensors (blood pressure cuff, digital stethoscope, medical imaging attachment), they can do remote exams too. If you don’t have the skills or tools, a nurse or aid can come to your home or workplace connect you all in a video conference with the remote expert(s).
As this trend continues, regulators must adapt and figure out how to handle licensing and oversight across state lines or international borders. Traditional States Rights will be challenged as our world becomes increasingly mobile and connected and where we change jobs and careers every few years and move about to exploit new opportunities. If we want to keep our health provider, how will that happen if she lives, and is licensed to practice, in another state?
 Healthcare Robots
Healthcare Robots
What if the person providing personal care at home is not a person at all but a robot instead? Japan, with its One Child per Family policy, faces a much more significant aging problem than we do, and they’re turning to healthcare robots for help. Japan is pioneering the early development of healthcare robots and hopes to have a robot in every senior’s home by 2015. That’s just 2 years from now. South Korea also faces an aging issue, as does most of the globe, and they’ve mandated a robot in every home by 2020.
They do this because robots can easily do repetitive tasks, or ones that are too dangerous or difficult for humans. They can easily lift and transfer heavy patients, but their strong arms lack sensitivity today. That will be fixed with improved sensors.
What’s especially attractive about robots is that they can work 24×7 without complaining about low wages or the lack of benefits; and while they’re expensive to buy now, those costs will fall as technology allows. Robots can be directed by humans or made to learn and operate on their own. And they can serve as personal assistants (e.g. Roomba vacuum or Paro companion robot seal), can be something we wear or ride in (e.g. exoskeleton or Google’s self-driving car), or even something inside our bodies (nano-scale bots in our blood stream).
 The Brain-Computer Interface
The Brain-Computer Interface
The ability to sense electrical activity of nerve endings is already leading to advanced prosthetics for amputees and so quadriplegics can control robot arms just by thinking about it. A brain-computer interface could also be used to control an exoskeleton or robot, and the military is already envisioning soldiers with telepathic helmets by 2020.
So what might be the result of converging Information and Cognitive Computing? Futurist Ray Kurzweil has studied this field and foresees a supercomputer exceeding the computational and analytically power of the human brain this year, in 2013. In many ways, IBM’s Watson already has. But by simply extrapolating Moore’s Law into the future, Kurzweil predicts that by 2023, a $1,000 computer will have the power of the human brain and by 2037 a $0.01 computer will too. By 2049 (still possible in my lifetime), a $1,000 computer will exceed the power of the human RACE, and ten years later a $0.01 computer will. Way before then we’ll see improvements in the brain-computer interface, so changes in healthcare beyond 10-20 years get much harder to imagine.
Update from Ray Kurzweil’s Predictions for the Next 25 Years (5/31/2015):
- By the late 2010s, glasses will beam images directly onto the retina. Ten terabytes of computing power (roughly the same as the human brain) will cost about $1,000.
- By the 2020s, most diseases will go away as nanobots become smarter than current medical technology. Normal human eating can be replaced by nanosystems. The Turing test begins to be passable. Self-driving cars begin to take over the roads, and people won’t be allowed to drive on highways.
- By the 2030s, virtual reality will begin to feel 100% real. We will be able to upload our mind/consciousness by the end of the decade.
- By the 2040s, non-biological intelligence will be a billion times more capable than biological intelligence (a.k.a. us). Nanotech foglets will be able to make food out of thin air and create any object in physical world at a whim.
- By 2045, we will multiply our intelligence a billionfold by linking wirelessly from our neocortex to a synthetic neocortex in the cloud. [Since I’m almost 67 now, this may happen in my lifetime if I live to 97.]
 The Most Likely Inhibitors
The Most Likely Inhibitors
As I mentioned at the beginning, politics and public policy can be either a huge driver of change or an inhibitor. So what I worry about most is the corrupting power of big money in politics and special interest lobbying. I’m appalled that most new bills today are drafted by corporate attorneys and not by elected politicians. Then highly-paid lobbyists help push the bills through Congress to become law.
Steven Brill, in his 38-page special report for TIME Magazine, described an immensely profitable healthcare industry that doesn’t want to change and spends twice as much on lobbying than the military industrial complex. If proposals such as universal healthcare were to actually eliminate the need for private health insurance and replace the profit motive with incentives to instead focus attention on wellness and prevention and thus avoid the need for medical care in the first place, the nation could easily save over $1 trillion per year. That’s each and every year, not spread over 10-20 years, and that would be a lot of money NOT pouring into the healthcare industrial complex.
No wonder the hospitals, insurers, drug companies, testing companies, and equipment providers have been fighting so hard to prevent real health reforms. Doctors themselves are less to blame, but even from their first day in medical school, they too have learned that preventative medicine kills – it kills repeat business, and profits.
GREED – and the widening gaps in income, wealth and opportunity – is a global problem, but it’s most pronounced in the United States. And unless we address this problem, we won’t be able to contain the rising healthcare costs and will continue paying more than all other industrialized nations for inferior care overall. Sure, the wealthy will get great care, but the others won’t.
About the Author
I want readers to know about the lens that makes up my perspective of healthcare and its future, so here’s some quick background. I’m a retired IBM technologist, market strategist, futurist, consumer advocate, and social entrepreneur. I started my professional career as a punch card operator with IBM while still in college. I progressed through computer operator, application & systems programmer, systems engineer, marketing support rep, and market strategist before retiring in 1999.
While I have no formal medical training, I have a fairly good basic understanding of the industry (not so much medicine itself) from my work as an IBM Systems Engineer with large hospital accounts, where I installed systems for patient accounting, patient care, pharmacy, and medical records. And I married a registered nurse (RN, BSN).
 I’ve always been interested in tech innovations and tend to think in IBM Scale, i.e. about big, multi-billion dollar problems.
I’ve always been interested in tech innovations and tend to think in IBM Scale, i.e. about big, multi-billion dollar problems.
About Modern Health Talk
After retiring from IBM, running a digital home consulting firm, and co-founding a 501(c)(4) nonprofit consumer advocacy firm representing homeowners in the Texas legislature, I started Modern Health Talk. I was looking for a compelling intersection of industry trends and market needs with my skills and interests, and that’s exactly where Modern Health Talk is positioned – at the intersection of several industry and market trends and positioned between online support groups on one side and technology websites on the other.
It’s a content website and blog with tools providing a personal assessment and product comparisons. There are lots and lots of healthcare statistics, many of which are packaged in nearly 300 infographics, and there are well over 400 articles on topics ranging from health reform to low- and high-tech solutions for home healthcare and aging-in-place.
Presentation Slides
Related Articles
By mousing over the Popular Keyword Tags in right sidebar, you can browse through nearly 100 articles on different aspects of the FUTURE, but I list my favorites here.
- The Future of Medicine Is in Your Smartphone, by Dr. Eric J Tool
- Aging and Brain Science
- Google Futurist Ray Kurzweil thinks we’ll all be cyborgs by 2030
- The Future of U.S. Healthcare, by Barry Bittman, MD
- Scientist sees aging cured, but who wants to live forever?
- The End of Illness
- Living in a Post-Human World (1:30min video, theoretical physicist Micheo Kaku says, “We will become the Gods we once feared.”)
- If you could live forever, would you? (1:30min video with Larry King and astrophysicist Neil deGrasse Tyson)
- Abbreviated Vision of the Future of Health Care
- Health & Medicine Outlook 2013
- Forecasts for the Future of Healthcare
- 10 Forecasts for the Future of Healthcare
- 11 Emerging Chronic Disease Technologies To Watch
- Medicine Unplugged: Your phone, your DNA, your data
- A Proposed Hybrid, Public/Private Model of Health Care
- A Totally New Healthcare System
- Innovator’s Prescription: Disruptive Healthcare Solution
- The Future of Medicine and Virtual Assistants
- What makes you sick? Ask Dr. Watson
- Big Data and the Future of Healthcare
- Will Robots Take Over in Health Care?
- Automation, Robots and The Pink Collar Future
- The Internet of Things: Prediction
- Telemedicine becoming the new house call
- TeleHealth: The Doctor Will See You Now, Remotely
- Is Telehealth the Future of Health Support?
- Are we Bringing Health Care Home or Sending it Overseas?
- The Smartphone Physical: Checkup of the Future?
- Smartphones are starting to bring Hospital Care Home
- The Nurse in Your Pocket
- A Doctor in Your Pocket: Future of Personalized Medicine
- Will mHealth be the Next Flight to the Moon?
- Wireless devices to change medicine
- The future of connected health devices
- MIT researchers use smart phones to monitor health
- 11 predictions for the Mobile Health market
- Under Skin Blood Test Sends Lab Results to Phone
- BioEnergy: Harvesting Power from the Body to Run Devices
- Mind control of helicopters now. What might be next?
- Printing Your Own Medicine… and Organs
- Does AI provide a Competitive Advantage?
- Teaching Computers to Hear Emotion
- High Tech Advancing Future of Personalized Cancer Care
- Bringing Dead Back to Life & Envisioning a Healthy Future
- How Wearable computing could take off
- Home Monitoring of Seniors will drive Wearable Devices
- Caregivers and the “Smart” Homes of Tomorrow
- Now the Real Work of Healthcare Reform Begins
- Healthcare Utility – Role of Government & Mobile Internet
- Do We Need Doctors Or Algorithms?
- Hospital-Insurer-Doctor lines start to blur
- Scientists exploring computers that can learn and adapt
- 10 Digital Health Trends for the Next 20 Years (72-slide presentation on Slideshare)
- Where Will the Century of Biology Lead Us?
- How Long Before I Can 3-D Print a Replacement Body for Myself? (The FUTURIST magazine)
- Where Will the Century of Biology Lead Us? (The FUTURIST magazine)
- The Future of Digital Health (SlideShare presentation by Monty Metzger)
- Mobile Health: Future of Mobile Health (SlideShare presentation by Monty Metzger)
- World’s Richest Doctor Buys World’s Most Powerful DNA Sequencer (with excellent 36-min video of NantHealth CEO Patrick Soon-Shiong discussing The Future of Medicine)
- Robot Brains Catch Humans in 25 Years, Then Speed Right On By (Bloomberg. I commented)
- Bionic Eyes Can Already Restore Vision, Soon They’ll Make It Superhuman (Gizmodo)
- What will happen when the internet of things becomes artificially intelligent? (Thought provoking)
- Healthcare’s Trillion-Dollar Disruption (Forbes, I commented)
- Will scientists wipe out disease by 2030 as Ray Kurzweil predicts? (San Diego Tribune. I commented)
- Why Tech is Accelerating (Huffington Post, I commented)
- What’s Next in Computing? (Great article. I commented)
- Artificial Intelligence Will Redesign Healthcare (MedicalFuturist.com)
- As Tech Trickles In, Medicine Is About To Hit Warp Speed (Great article in Digital Trends)
- The world in 2045, according to Pentagon researchers (World Economic Forum)
- Driverless ambulances and drone doctors: The hi-tech future of healthcare revealed (DailyMail.com)
- The Top 10 Trends Shaping the Future of Pharma (MedicalFuturist.com)
Related Video
Related Infographics
- The 40 Trends Driving the Future of Medicine (MedicalFuturist.com)
- The Future of Healthcare+
- The Future of HealthTech
- Envisioning the Future of Healthcare
- Future: Tomorrow Starts here
- Big Data and the Future of Healthcare
- The Future of Health is in your Smartphone
- Will Virtual Assistants Propel the Future of Medicine?
- The Future of Electronic Medical Records
- What’s Possible for Health Care?
- The Digital Diagnosis


With 25,000 times more storage capacity, a modern thumb drive sells for just $18, compared to the $3,200/month that IBM leased its storage system for in 1956.

Can America’s Fastest Supercomputer Defeat Covid for Good? (Popular Mechanics, August 2021) “The nation’s brightest computer scientists were pressing Summit, a 200-petaflop supercomputer, into service as a Covid-fighting machine. The only problem? They had to keep the machine — which demands constant monitoring from a crew of on-site technicians — running, despite a global pandemic.”
As a retired IBM technologist now writing about healthcare policy, I found this article fascinating. It describes how AI, machine learning, and the incredible compute power of 200 quadrillion operations per second is helping to defeat the pandemic. But I was intrigued by the intro, which described the critical nature of infrastructure and how important it was to keep this supercomputer running.
AND LOOKING BEYOND 2020
10+1 Medical Technologies that Blew My Mind (The Medical Futurist) — In this video (9:58), Dr. Bertalan Mesko, MD, presents his view of the 10(+1) technologies that blew his mind and made him feel like we’re entering an era that belongs to science fiction movies!
1. 3D printed drugs
2. Smartwatch ECG
3. Portable Ultrasound
4. Mixed Reality
5. Digital Twins
6. Sleep tracking and smart sleep alarm
7. Digital Pills
8. Medical Drones
9. Genome Sequencing
10. At-home lab tests
10+1. A.I. in public health
MORE RELATED 3RD PARTY ARTICLES:
Survival of the richest: The wealthy are plotting to leave us behind (CNBC Technology) I found this incredibly thought-provoking article to be a perfect blend of two disturbing trends:
1. The Exponentially Accelerating Pace of Tech Innovation, which I hint at in Moore’s Law and the FUTURE of Healthcare, brings with it concerns over how humans will be able to control and govern whatever technology brings us.
2. The Widening Wealth Gap further brings with it the corrupting influence of big money in politics.
As the author shared his experience and thoughts from meeting with a handful of user-wealthy global oligarchs, I became more convinced that my own fears are more than justified. I’ve been writing for a while that the biggest problem I see is government’s inability to understand, regulate, and control markets and products resulting from tech innovation. Instead of speeding the process of lawmaking, it seems to have come to a halt and is even falling backwards in the name of conservatism and preserving “the good ole days.”
The Heart of The Matter: Technology In The Future of Cardiology (The Medical Futurist) COMMENT: As sensors and medical devices keep getting cheaper, smaller, more accurate, and easier to use, more and more medical functions will move down-market from physicians in clinics to consumers at home or on the go. This trend could completely disrupt many of today’s business models and help lower the overall cost of providing healthcare. After all, “An ounce of prevention is worth a pound of cure.”
What Kids Need to Learn to Succeed in 2050 Focus on the 4-Cs: Critical Thinking, Collaboration, Communication, and Creativity.
Your iPhone could handle 120 million moon missions at once (7/16/2010)
Stanford University finds that AI is outpacing Moore’s Law (Computer Weekly, 12/12/19) While Moore’s Law maps out how processor speeds double every 18-24 months, the speed of artificial intelligence computation doubles every 3 months, according to Stanford’s 2019 AI Index report.
The hospital is dead, long live the hospital! (excellent McKinsey & Company report)
What it’s like inside the doctor’s office of the future (C|Net, 5/23/19) For $149 a month, Forward Health’s futuristic health center wants to replace your primary care clinic.
Artificial Intelligence will Crush Humans, “It’s not even close.” (Futurism.com 5/17/21) Nobel Prize winner Daniel Kahneman said, “In the battle between AI and humans, it’s going to be an absolute blowout — and humans are going to get creamed.” How people adjust to this will be interesting.
What about the Future of Moore’s Law itself?
According to this C|NET article, IBM is spending $3 billion to push the far future of computer chips. Among the technologies being explored are Quantum computing, Neurosynaptic computing, Carbon nanotubes, Silicon photonics, Tunnel field effect transistors, Graphene, and III-V materials. But with so many, will that water down the $3B investment?
Will scientists wipe out disease by 2030 as Ray Kurzweil predicts? (I commented)
Is Exponential Acceleration Part of Evolution? (I commented)
The FUTURIST Magazine features an interesting article by Dr. Bertalan Meskó (http://www.wfs.org/futurist/2014-issues-futurist/may-june-2014-vol-48-no-3/rx-disruption-technology-trends-medicine-and) that includes an infographic showing various trends that are already available to healthcare practitioners or patients and those that still need time to develop.
Think Like a Futurist to Be Prepared for the Totally Unexpected Wall Street Journal article about the art and science of suturing, which is fast becoming a necessary skill, and where we read signals, see trends and ruthlessly test our own assumptions.
How the future of medicine lies in cells (CBS News features interesting research into stem cells)
Scientists Created The First Nanorobots Programmed To Destroy Cancer Tumors (ThinkingHumanity)
CRISPR: The gene-editing tool revolutionizing biomedical research (CBS News) This new tool could be the key to treating genetic diseases and may be the most consequential discovery in biomedicine this century.
How Big Tech Is Going After Your Health Care (NY Times) Apple, Google, Microsoft and other giants are accelerating their efforts to remake health care with new tracking apps, sensors and other tools.
How Alphabet, Amazon, Apple, and Microsoft are shaking up healthcare — and what it means for the future of the industry
The 8 Healthcare Predictions for 2019 (Forbes)

This is the time of year when everyone seems to make technology forecasts. I’ll post those I find interesting, starting with:
The Future of Vision and Eye Care (Medical Futurist, Oct.2019) With more than 80% of our perception coming from vision, this article covers the future of remote diagnostics, augmented reality, digital and 3D printed contact lenses, bionic eyes, artificial retina with brain implants, gene therapy, artificial intelligence, and more. In my own view, I can envision night vision and even “seeing” infrared and ultraviolet light or radio waves.
The Future Of Hearing: How Technology Might Turn Us Into Superheroes (Medical Futurist, Oct.2019) “The appearance of hearing and ear-based technologies, such as headphones, earbuds, hearing aids, and many other devices that measure health parameters via the ear – with a common term: hearables – signify a new age for treating hearing-related health troubles. These devices can combine multiple functions, can be used for diagnostics or treatment, and often feature innovative solutions in style, color, and accessibility.”
The Age of Surprise: Predicting the Future of Technology (FORBES)
Google’s chief futurist Ray Kurzweil thinks we could start living forever by 2029
How the “Internet of Things” will replace the web
Envisioning the Future of Health Care After my own perspective, Cleveland Clinic CEO Toby Cosgrove shares his view that the primary emphasis should be on wellness & prevention programs, like for smoking & obesity, along with efficiency improvements to our delivery system. I certainly agree.
McKinsey&Company questions the future of Moore’s Law They did an in-depth analysis, but I don’t think they gave enough consideration of new technologies that will replace semiconductors, including quantum computers, organic computers, and DNA storage, each of which would likely Accelerate Moore’s Law, not slow it.
DNA: A New Approach to Information Storage
Scientists reverse aging process in mice.
In this 17 year old video, a science icon warns about the need to be knowledgable and skeptical about science and technology and to ask the tough questions of ourselves, our children, and our leaders. Otherwise we abdicate control to those who may not have our best interests in mind.
4 Crazy Predictions For The Future Of Health Care: Human Augmentation, Hacked DNA, And More (FastCompany, I commented)
7 Top Futurists Make Some Pretty Surprising Predictions About What The Next Decade Will Bring
This Huffington Post article includes predictions about:
(video interview at Exponential Medicine
Investing in the Future of Healthcare with Vinod Khosla (video interview at Exponential Medicine
Here’s How IBM Watson Health Is Transforming the Health Care Industry I commented:
IBM Predicts 5 Life-Changing Innovations for the Next 5 Years
Not all health care technology raises costs. By using automated methods to collect and track laboratory test results, Patient Engagement Systems improves the care of patients with diabetes and other chronic conditions and lowers costs by $2400 per patient per year. The benefits come by connecting these patients (who are among the most expensive to care for) to the most efficient and high-quality source of care – their primary care providers – and avoiding the need for Emergency Room and hospital visits. This digital “ounce of prevention” brings a solid “pound of cure” for patients, providers and payers.
The Patient Engagement approach takes advantage of existing infrastructure and the tenets of Behavioral Psychology to yield benefits that are proven by published trials as well as real-world experience with thousands of patients.
Thanks for your excellent essay and for keeping these important issues front and center.
Benjamin Littenberg, MD, Chief Medical Officer, Patient Engagement Systems
MIT Technology Review today published “We Need a Moore’s Law for Medicine.” I commented…
I find the timing of this article interesting, since I published “Moore’s Law and the FUTURE of Health Care” just over a month ago. (https://www.mhealthtalk.com/2013/07/moores-law-and-the-future-of-healthcare/) But I’m not complaining and instead applaud any article that promotes beneficial uses of technology and exposes the challenges of adopting them appropriately. One of the obstacles I noted in my paper was Greed and its influence on public policy.
Americans spend nearly twice as much as other industrialized nations but live sicker and die younger (per WHO), so we “should” be able to cut our $2.7+ trillion annual healthcare expenditures in half, saving over $1 trillion per year. That’s each and every year, not spread over 10-20 years, but that would be a lot of money NOT pouring into the Medical industrial complex.
The Healthcare industry, including hospitals, insurers, drug companies, testing companies, and equipment providers, is immensely profitable and spends twice as much on lobbying as the Military industrial complex to keep its revenues flowing. So while savings from applied technology or changes to business models seem reasonable, strong opposition opposes real change.
Elon Musk Claims We Only Have a 10 Percent Chance of Making AI Safe (Futurism.com) Be sure to watch the embedded TED Talk. It’s chilling.
COOL EXAMPLES:
Check out this list of The 14 Most Innovative Gadgets of All Time.
1. Microsoft Kinect (With gestures, You are the controller.)
2. Sony Walkman (People started carrying their music with them.)
3. MakerBot Replicator (3D print almost anything: food, clothing, even other machines)
4. Google Glass (1st wearable heads-up display to grab public’s attention in big way)
5. iPhone (integrated device with no buttons that changed mobile device design)
6. iPad (made tablet computers desirable)
7. NEST (smart thermostat learns your habits)
8. Google Self-driving Car (great for seniors when they can no longer drive)
9. Connected TVs (stream Netflix, Hulu, HBO Go, Amazon Instant, YouTube)
10. Solid State Drives (boots faster than hard disks)
11. Cloud Computing (collaborate with no need for backups)
12. SIRI (voice-controlled assistant learns)
13. LTE Phones & Tablets (high-speed wireless Internet)
14. Bendable Displays (thin & flexible for your pocket)
Here are 10 Innovative Health Gadgets from CES:
1. Scanadu Scout (billed as a medical tricorder, senses vitals)
2. Basis B1 Watch (tracks heart rate, perspiration, skin temp)
3. Fitbit Flex (wristband pedometer syncs using Bluetooth 4)
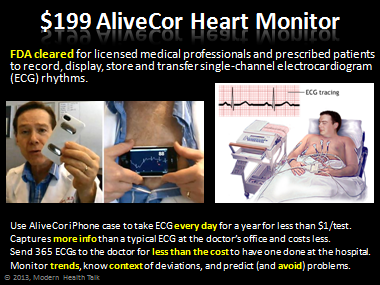
4. AliveCor Heart Monitor ($199 FDA-approved ECG for iPhone)
5. Wahoo Fitness Blue HR Heart Rate Strap (syncs w Bluetooth 4)
6. HAPIfork (tracks eating habits, helps improve behavior)
7. LUMOBack Posture Sensor (vibrates when you slouch)
8. Withings Scale (tracks weight, heart rate, body fat, BMI)
9. ibitz Activity Monitor (activity tracker for kids)
10. iRiver ON Fitness Monitoring Earbuds (activity, heart rate, calories burned)
A WORD OF CAUTION:
Are you a bit paranoid about the possibilities? Maybe you should be since cool medical technologies can be used for good, or evil. The FDA has already approved a digital pill by Proteus that’s powered by enzymes in the stomach and then communicates to a smartphone via a patch worn on the abdomen. That’s cool, but here’s a video about possible uses of Electronic Tattoos or Ingestible Pills that go beyond their initial intent. And here’s a longer and scarier video. Both were produced to make you paranoid and fear tech innovation. They present an entirely feasible scenarios of possible futures, but that’s exactly why futurists need to consider all scenarios and help society plan for the preferred version.
My point is NOT to scare you but to suggest that it’s entirely possible that good public policy may not be able to keep up with the accelerating pace of tech innovation. Bad policy, however, may keep up and even accelerate innovation if large profits or national security are at stake.
Humans Need Not Apply (YouTube)
This is an interesting video that shows automation of information processing (brains, thinking & learning) occurring much faster than previous automation of manual labor (muscles). And it’s happening at an exponentially accelerating rate. (See https://www.mhealthtalk.com/moores-law-and-the-future-of-healthcare/)
What will happen as more and more jobs are automated and humans, who are living longer, become obsolete? What societal issues will arise?
Should societal issues caused by AI & automation be left to politicians to resolve, and a political process corrupted by special interests? Will the pace of their policy-making be able to keep up with the pace of tech innovation? (It’s already slowing with our divided Congress, as technology speeds up.)
So while our Constitution starts with “We the people,” I must today ask, “Who are ‘WE’?” We can begin answering that question with our vote – for either a united nation of diverse nationalities and beliefs, or a divided nation of warring tribes ruled by rich white men in suits.
I commented on the video at YouTube.com: