TeleHealth: The Doctor Will See You Now, Remotely
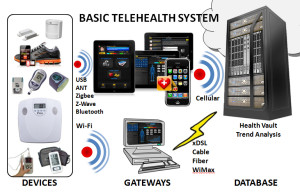
There’s a fairly new option for after-hours medical care that connects you with practitioners anytime, anywhere. It’s called Telehealth or Telemedicine, and it’s offered by companies like American Well, MyNowClinic, and OptumHealth.
Hospitals already use high-speed Internet connections to share medical information among specialists within the facility or in different locations. And they can even put a rural patient in front of a big city specialist miles away. But as Internet use permeates people’s everyday lives, health care professionals are able to connect with patients in real time over any distance without traveling or scheduling an office visit. Previously when you were sick, you had to go to the doctor. Now she can come to you, electronically 24/7. Some services also provide in-home visits by physician assistants to supplement telehealth.
“While having access to a doctor outside of normal office hours is a popular telehealth service, it isn’t the only one. Doctors can also monitor the vitals of chronically-ill patients in real time and will be able to adjust medicines or treatments without requiring the patient to come in,” says Jonathan Linkous, chief executive of the American Telemedicine Association (ATA).
Read more at http://www.foxbusiness.com/personal-finance/2011/08/30/telehealth-doctor-will-see-now-wherever-are/.
Extending Telehealth to Consumer Households – Wayne’s views
Modern Health Talk founder Wayne Caswell has been following and contributing to several telehealth discussions in Linkedin groups. Here are highlights from one of those discussions:
Poly,
Thanks for referencing my article on Extending Telepresence & Telemedicine to Patients’ Homes and for writing me directly to ask me to participate in a discussion of “How do you think telehealth developments will impact seniors and less-mobile patients?” There’s too much to say here, so I’ll just summarize key points and capture details later in a paper I’m writing with a retired orthopedic surgeon who gave up his practice to focus on telemed. Still, it’s a long post. ‘Sorry about that.
- POLITICS & INCENTIVES – As a nation with the highest healthcare costs, at over $2.4 trillion per year and rising rapidly, what will the political climate allow? Are we going to focus on reducing costs or maximizing profits? Much of the industry will fight to preserve their pay-per-procedure cash cow, which arguably leads to waste without results. New ACO models aim to reduce unnecessary tests & procedures, prevent returns to hospitals, and coordinate care among specialists, but the industry still has a built-in incentive to treat symptoms rather than provide cures and promote wellness. Lobbyists for powerful special interests want to keep it that way, and so do many private practice physicians.
- MEDICAL ETHICS – Healthcare debates often involve tough issues of medical ethics, especially when we have personal control over half of the factors determining our health but so many people still smoke, drink or eat too much of the wrong things. Obesity, which increases with age, is America’s #1 health and financial risk, bar none. It’s known to cause heart disease, stroke, diabetes and certain cancers, and we’re on track to see half of our population overweight. Should diabetics get the same level of care? As a voting bloc, they’d say yes.
- DIGITAL DIVIDE – Technology and the Internet are keys to telemedicine, telework, distance learning, e-commerce, and e-government, but the latest FCC report to Congress says a full one-third of U.S. households lack broadband access. That’s either because they have no access to it or because it’s too expensive or they lack the skills or perceived need. So, is telemedicine to focus on the lowest common denominator (voice telephony) or on the latest in high-definition telepresence? And are we willing to write-off entire sectors of our population and give them inferior care because they’re poor, black, Hispanic, elderly, live in rural communities, and don’t have broadband Internet access? Or are we going to fund computer literacy and universal access to broadband? Which is cheaper or better for the nation?
- FITNESS – People who have focused on their own well being and invested the time and money in healthy diet, exercise and routine checkups will naturally resent having any of their taxes go toward healthcare for those who drink or smoke excessively, are obese, or live otherwise risky lifestyles. I’m not sure what it will take to get their votes when the times comes.
- AGE – We as a society feel a responsibility to fund the healthcare needs of young soldiers returning from war without limbs, even if it means spending hundreds of thousands of dollars for bionic arms and legs and rehabilitation. Such expenses seem justified to help them contribute to society and to lessen long-term care costs. But what about the elderly? It somehow seems less justified to spend so much on their end-of-life care due to escalating costs with age and the fact that they’ve come to the end of contributing to society. So, on one hand it seems prudent to fund the VA and less so to fund Medicare, but seniors also make up a powerful voting bloc.
- LONG TERM CARE – The average lifespan when Medicare & Medicaid were enacted was 67, so Medicare kicked in at age 65. That way it would last just two years. But people don’t want to change that start date even though the average lifespan is now 78 and could soon exceed past 100. It’s not just about federal funding, however. Healthcare costs balloon in the last months of life, often with procedures that are either medically unnecessary or unwanted by the patient, but proposals to fund End-of-Live counseling were politicized as “death panels.” Just 9% of adults age 65-69 need daily care, but 50% of those 85+ need care.
- INCOME – As a society, we tend to look down on the poor and unemployed and blame them for their own plight – at least some in our society do. That’s unfortunate, because certain social classes have been put there and kept there and have fewer opportunities to improve themselves. They have fewer educational opportunities, job opportunities and even the ability to eat right. Many inner city neighborhoods, for example, lack grocery stores with fresh produce, and residents there find processed foods cheaper. And without a full-time job that provides health insurance and the means to pay for their own insurance, they don’t get preventive care and rely instead on higher-cost emergency care when needed.
- HOME CARE – The nation could save over $1 trillion per year by moving at least half if its healthcare from institutions to homes, but current funding models (Medicare, Medicaid and private insurance plans) don’t support long term care. And since Medicaid only pays when you’re poor, you first have to become poor and be put in a nursing home, which costs four times that of home care. Modern Health Talk focuses on technologies for home healthcare.
- REGULATION – Has HIPAA gone too far? Should it extend to the transmission of medical data or just the storage of it? Do we really need HIPAA-certified home gateways and video conferencing products? Isn’t video conferencing just an extension of a phone call? We don’t have HIPAA phones. Similar issues relate to new FDA proposed rules for mhealth devices, and I can argue that reliability of the telecom network is as important as the reliability of medical sensors, especially if the sensor alert never reaches the remote monitoring service due to QoS issues.
- OUTSOURCING (added 9/13/11) – Get ready for outsourced health care. Broadband Internet connections to India are often faster than to Indiana, and that makes it easy to outsource knowledge-based jobs to countries with lower wages. We’ve already seen examples of “Sun, Sand & Surgery” vacations for major operations at lower cost, but how will society react when that concept extends to telehealth for everyone – at lower cost with practitioners in Bangladesh? How might those services be regulated? But what about the doctors here?
- SECURITY – Privacy is one issue, but security is another, whether that’s protecting data stored locally or in the cloud. Recent data breaches show that many hospitals are not ready to shift to electronic records. That’s one reason I’ve been inserting myself into telehealth discussions: I have a strong IT and security background from my years as an IBMer, consultant, and member of the FCC Consumer Advisory Committee. At the FCC I served on three working groups: (1) advanced technology, (2) homeland security and (3) rural and under-served communities.
- FAMILY – Are we going to find a way to compensate unpaid family caregivers who spend an average of 22 hours/week carrying for loved ones and help ease their burden? That burden totals $450B/year in lost worker productivity, reduced earning capacity & retirement income, and increases in their own physical & emotional health. That’s about 3.2% of the U.S. GDP in 2009.
- RENT VERSUS BUY – Equipment Rental models can make more sense for short-term needs while recuperating from an illness or during hospice, and Purchase models can make more sense for fitness, wellness and long-term care, especially when multiple parties are part of the care plan, including doctor, patient, family advocate, and paid caretaker.
- HEALTH GATEWAYS – What device will interface between remote monitoring services and in-home (or mobile) medical and environmental sensors? Will it be a PC, tablet, smartphone, specialized device or a TV set-top box? There’s likely no one answer and the choice may depend on (1) the rent/buy model and (2) the need to interoperate with other subsystems (home security, HVAC, lighting, surveillance, electronic door locks, etc.).
- BEHAVIORS – Ethnographic market research is needed to better understand daily tasks & behaviors of disabled or frail patients and their caretakers, as well as the challenges they face adopting tech solutions.
- AWARENESS – Modern Health Talk was established to help address the low public awareness and understanding of home care technology.
For telehealth to truly work, I think that all of the issues I’ve presented need to be addressed at once. What do you think? Leave a Reply below.


In Spurring the market for high-tech home health care, the authors observe that “A daunting array of financial and operational barriers is holding back growth” and asks “What can be done?” The report was published September 2011 by consulting firm McKinsey. It’s very well written but needs registration to see the whole thing. Here’s my summary and added insight:
Spurring the market for high-tech home health care
by Basel Kayyali, Zeb Kimmel, and Steve van Kuiken
McKinsey describes the goal of high-tech home health care as preventing or reducing the need for institutional care, alleviating the financial and emotional burden upon society and individuals. They described how clinical or economic factors can propel seniors from one care setting to another.
* Declining mental or physical health often cause the shift from homes to assisted-living facilities.
* Medical events such as falls and heart attacks can cause a shift from homes or assisted-living to acute-care institutions.
* Movement across a financial or clinical breaking point (e.g. bankruptcy or diagnosis of dementia) can prompt a shift to long-term care institutions such as nursing homes.
While McKinsey argues that technology-enabled home health care should be thriving in the U.S., we should realize that the enabling technologies are just now becoming available with a price point and ease of use to attract attention. Because it’s so new, awareness remains an issue, which is why I founded Modern Health Talk.
Many of McKinsey’s cited financial and operational barriers complement the issues that I list in the article above. Chief among them are:
* misalignment of incentives between payers and providers, where every patient successfully kept at home means less revenue for the hospital. One way to accelerate the alignment of incentives is with Accountable Care Organizations (groups of coordinated health care providers)
* strong and proven value proposition among clinicians and patients alike.
* “closed feedback loop” to measure progress against goals, prove the technology’s value, and measure and optimize it.
* usability suitable for the target audience
* repetition such as daily use of an electronic weight scale that becomes habit, compared to an annual eye exam that’s less compelling for home use.
* fraud prevention mechanisms
McKinsey then compares health care incentives in developed versus developing nations, suggesting that the former is mostly interested in containing rising costs while the latter is interested in extending care to underserved communities. I understand where they’re coming from but disagree and look at bridging the U.S. Digital Divide as a key benefit of telehealth and mhealth initiatives. That’s why I also advocate for programs that extend broadband Internet access to rural areas.